24-Hour vs. Live-In Care: What's Best?

Choosing between 24‑hour care and a live‑in caregiver in Philadelphia means balancing around‑the‑clock supervision with the benefits of a single, consistent caregiver — and thinking about cost. This guide explains how each model works locally, why those operational differences matter for safety and independence, and which payment and program options in Pennsylvania can affect your decision. You’ll find clear indicators (medical, cognitive, and environmental) that point to one model over the other, typical cost ranges, and local resources to explore. We also map key features and trade‑offs, compare overnight policies, break down common cost elements, explain how dementia or mobility needs change recommendations, and summarize Pennsylvania‑specific programs and regulations. Read on for side‑by‑side comparisons, practical checklists, and straightforward guidance to help you choose the right in‑home care plan for your loved one in Philadelphia.
What Is 24‑Hour Home Care in Philadelphia?
In Philadelphia, 24‑hour home care means arranging in‑home caregiving so a client has continuous coverage day and night — usually through rotating awake shifts or overlapping staff. This model provides real‑time supervision, reliable medication support, and immediate response to falls or behavioral crises, making it a fit for people who need constant monitoring. Agencies commonly staff several caregivers in shorter, awake shifts or paired schedules; some private hires use alternating caregivers to cover the same hours. Knowing how staffing and monitoring are organized helps families compare safety outcomes and cost implications. Below, we outline the main features and benefits families see with continuous 24‑hour coverage. For a full list of the caregiver services we provide, explore our website.
What Are the Key Features and Benefits of 24‑Hour Care?
Twenty‑four‑hour care offers continuous supervision, structured medication oversight, and fast emergency response — a combination that lowers the chance of adverse events for high‑risk clients. Having trained staff present reduces fall risk by allowing prompt assistance during transfers and nighttime toileting, and it supports complex medication schedules and medical device management. Families frequently report greater peace of mind and fewer hospital readmissions when constant supervision matches clinical need. For example, a Philadelphia household caring for someone with frequent nighttime confusion may avoid repeated ER trips by arranging awake overnight coverage. Those safety and continuity benefits naturally lead to the practical question of cost and affordability.
How Much Does 24‑Hour Home Care Cost in Philadelphia?
Costs vary depending on care intensity, whether you hire through an agency or privately, and whether the coverage uses multiple awake shifts or a live‑in caregiver with overnight checks. Citywide averages convert hourly caregiver rates into daily or monthly estimates based on the chosen model. The table below breaks down common cost components and typical ranges to help families budget and compare options.
This table shows typical cost components for continuous home care in Philadelphia:
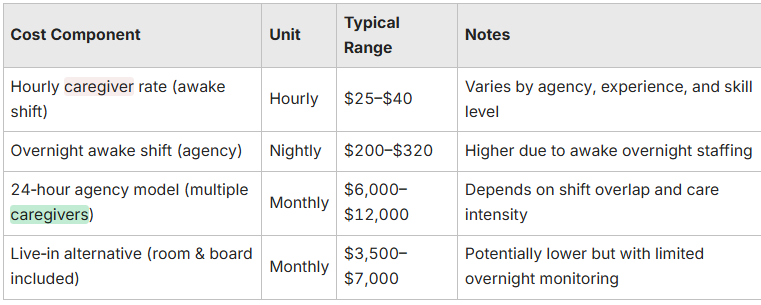
This breakdown highlights typical ranges and shows that specialized dementia training or skilled nursing needs can raise costs. Next, we’ll explain how live‑in care differs in structure and expectations so you can weigh safety and continuity against these price patterns.
For guidance tailored to your household and clinical needs, families can request a consultation with Home Matters to compare 24‑hour home care models and alternatives that fit their situation. Learn more about our commitment to compassionate care on our About Us page.
What Is Live‑In Care in Philadelphia?

Live‑in care in Philadelphia means one caregiver resides in the client’s home and provides daily assistance and companionship while taking scheduled rest or sleep breaks at night. This model prioritizes continuity: the same caregiver handles most daytime tasks — personal care, meals, errands, and social engagement — which builds routine and a deeper caregiver‑client relationship. Live‑in arrangements usually include periods when the caregiver is off‑duty or asleep, which affects overnight responsiveness and risk management. Understanding these trade‑offs helps families judge whether consistent daytime support and often lower base cost outweigh the need for immediate overnight supervision. The next subsection clarifies typical live‑in roles and expectations so you can assess fit.
What Are the Roles and Expectations of Live‑In Caregivers?
Live‑in caregivers typically assist with personal care, medication reminders, meal preparation, light housekeeping, and companionship while living in the client’s home with agreed private space and rest times. Best practice includes a written agreement that spells out work hours, sleep‑break norms, wages, and boundaries between caregiving duties and household tasks to protect both parties. Many families also document on‑call expectations and emergency procedures so everyone knows overnight responsibilities and escalation steps. Clear boundaries and a formal schedule help preserve caregiver wellbeing while maintaining reliable continuity of care for the client. You can find a comprehensive overview of our caregiver services on our site.
How Much Does Live‑In Care Cost in Philadelphia?

Live‑in care often costs less per month than multiple awake‑shift 24‑hour models because a single caregiver’s pay plus room and board can be more affordable than agency staffing. Typical monthly ranges depend on caregiver experience, neighborhood cost of living, and whether an agency handles payroll, taxes, and supervision. Families should budget for base pay, legally required wage considerations, and any overtime or extra coverage if a caregiver provides extended awake overnight shifts. Comparing live‑in estimates to awake‑shift 24‑hour costs helps determine which model fits your safety needs and budget.
Below is a short row comparison showing common live‑in cost elements:
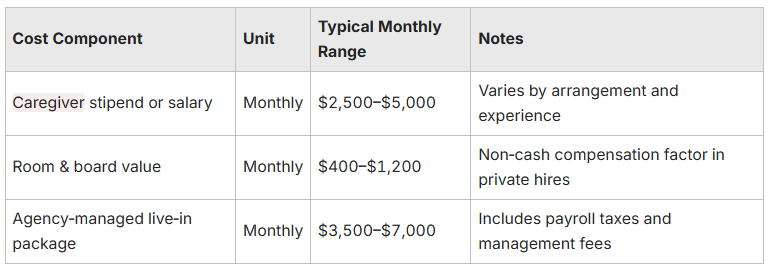
This snapshot explains why many families prefer live‑in care when daytime continuity is most important and immediate overnight response is less critical. For families weighing local pricing, Home Matters can provide a tailored consultation to compare live‑in and 24‑hour awake‑shift options and estimate likely costs for your Philadelphia neighborhood.
What Are the Key Differences Between 24‑Hour Care and Live‑In Care?
The main differences come down to caregiver presence, overnight sleep policies, cost structure, and continuity — all of which affect safety and long‑term suitability. Twenty‑four‑hour care usually relies on multiple caregivers working awake shifts to ensure active supervision; live‑in care uses a single caregiver who sleeps on site with scheduled breaks. Because awake overnight coverage requires more staffed hours, agency fees tend to be higher, while live‑in models can be less costly but may leave overnight gaps. Comparing these attributes against a client’s medical needs, cognitive status, and home layout helps families choose the safest, most sustainable option. The table below summarizes these points for quick reference.
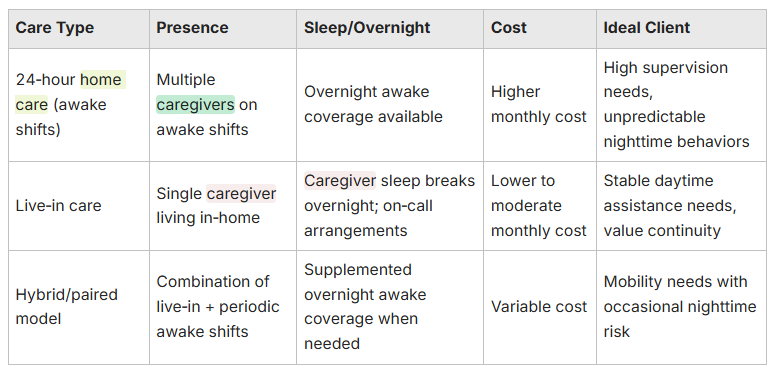
This side‑by‑side comparison clarifies major distinctions and helps families match a model to clinical indicators and budget realities. Below we unpack how presence and sleep requirements influence safety and caregiver fatigue.
How Do Caregiver Presence and Sleep Requirements Differ?
Awake‑shift 24‑hour models provide continuous monitoring and faster response to falls, wandering, and medical events because staff are scheduled to be awake and hand responsibility off at shift change. Live‑in care depends on proximity and agreed sleep breaks, which can leave limited overnight monitoring unless you add technology or supplemental awake shifts. Sleep arrangements affect caregiver alertness, staff retention, and legal liability: caregivers working frequent, interrupted nights are more likely to experience fatigue, while scheduled awake shifts protect rest but introduce multiple caregivers into the household. Those practical differences help determine which model reduces risk for clients with nighttime needs.
What Are the Pros and Cons of 24‑Hour Care vs. Live‑In Care?
Here are balanced lists of typical advantages and trade‑offs for each model to help you align clinical priorities with resources.
Pros of 24‑hour care:
- Continuous awake supervision lowers immediate risk from falls and nighttime crises.
- Agency oversight often includes training, back‑up staffing, and clear supervision.
- Scheduled shifts help protect caregiver rest and reduce fatigue.
Cons of 24‑hour care:
- Higher monthly cost can be a barrier for many families.
- Multiple caregivers may reduce continuity and relationship building.
- Shift handoffs can create occasional coordination challenges.
Pros of live‑in care:
- Single‑caregiver continuity supports stronger relationships and consistent routines.
- Often more affordable for steady daytime assistance needs.
- A familiar caregiver may notice subtle changes in health or function sooner.
Cons of live‑in care:
- Overnight monitoring is limited unless you add technology or extra shifts.
- Without clear agreements, caregiver fatigue and boundary issues can arise.
- Private hires add employer responsibilities (payroll, taxes) for families.
Because of these trade‑offs, many families try hybrid options or short trial periods before committing to a long‑term plan. Discover why Home Matters for comprehensive in-home support. Next is a decision framework to guide your selection.
How Do You Choose Between 24‑Hour Care and Live‑In Care for Your Loved One?
Choosing a model requires a structured assessment of safety, medical needs, cognitive status, budget, and the home environment. Start with an objective needs assessment — looking at nighttime behaviors, mobility, medication complexity, and family availability — then use trial periods and regular reviews to confirm fit. Involving medical professionals, social workers, or a care manager helps translate clinical indicators into a recommended plan. Below is a prioritized checklist and clear steps families can follow to decide with confidence.
What Factors Should Influence Your Choice?
Use this prioritized checklist to align needs with the right model. Start with safety, then consider routines and cost.
- Medical and cognitive needs: Does the person have unpredictable nighttime behaviors or complex medication schedules?
- Fall risk and mobility: Is frequent physical assistance required for transfers or walking?
- Family availability: Can relatives cover nights or provide regular respite, or is professional overnight care needed?
- Budget and payment options: What funding sources are available and what can the household sustain long term?
- Home layout and accessibility: Are bedrooms, bathrooms, and entrances arranged to enable prompt caregiver response?
Putting safety first helps families avoid models that leave critical gaps and leads into clear indicators for when 24‑hour care is the safer choice.
When Is 24‑Hour Care More Suitable Than Live‑In Care?
Twenty‑four‑hour care is usually recommended when someone has severe dementia with nighttime wandering, frequent falls or transfers that require assistance, complex medical regimens needing immediate response, or a recent hospitalization that raises complication risk. Signs that point to awake overnight coverage include repeated nighttime calling, a current history of falls, dependence on oxygen or complex devices, and unpredictable behavioral episodes. Short vignettes — for example, an older adult who repeatedly leaves the bedroom at night — show why awake overnight supervision can substantially reduce emergency visits. Spotting these signs early helps families choose the model that prevents avoidable hospitalizations.
How Does Specialized Care Affect 24‑Hour and Live‑In Care Options in Philadelphia?
Specialized needs like dementia or significant mobility limitations change staffing, monitoring intensity, and required caregiver training for both 24‑hour and live‑in care. Dementia care often benefits from continuous supervision and staff trained in behavioral de‑escalation and structured routines; mobility care requires caregivers skilled in safe transfers and fall prevention. Agencies that provide dementia‑trained staff or enhanced mobility training will influence both cost and safety. Ask providers about caregiver credentials, dementia training, and experience with assistive equipment when evaluating options. The subsections below explain dementia‑specific benefits of 24‑hour care and how live‑in care can support people with mobility challenges.
What Are the Benefits of 24‑Hour Care for Dementia Patients?
For people with dementia, 24‑hour care reduces wandering, enforces consistent routines, and lets trained staff intervene quickly during agitation or confusion. Continuous presence allows caregivers to manage medication reliably, use orientation cues to reduce sundowning, and respond to behavioral fluctuations before they escalate. Structured routines delivered by trained teams can lower safety incidents and hospitalizations. Clinicians often recommend continuous coverage for high‑risk dementia cases because it improves crisis management and overall safety.
How Does Live‑In Care Support Individuals with Mobility Challenges?
Live‑in caregivers provide steady daytime support for transfers, use of mobility aids, guided exercise routines, and adherence to physical therapy — all of which help preserve function and prevent deconditioning. A consistent caregiver can improve coordination during transfers and encourage regular activity. However, live‑in models may leave nighttime gaps for people prone to falls; pairing live‑in care with monitoring technology or periodic awake overnight shifts can offer a safer balance. Combining daytime continuity with supplemental overnight coverage often works well for people with mobility limitations who don’t need constant nocturnal supervision.
What Local Resources and Regulations Affect Home Care Services in Philadelphia?
Philadelphia families should factor in Pennsylvania programs, veterans’ benefits, and state labor rules that affect affordability and legal obligations for live‑in arrangements. Public options — like Medicaid home‑and‑community‑based services waivers and VA programs — can offset some private‑pay costs, though eligibility and benefit levels vary. Pennsylvania labor and health regulations cover wage, overtime, and employer responsibilities families must understand before hiring live‑in caregivers directly. Local support groups and community resources can supplement paid care with respite and caregiver education. For additional guides and helpful information, visit our resources page. The subsections below summarize the main programs and regulatory points relevant to Philadelphia decision‑making.
What Government Programs and Financial Aid Are Available for Senior Care in PA?
Several state and federal programs often interact with in‑home care financing in Pennsylvania, including Medicaid waivers for home‑and‑community services and veteran‑directed care or other VA benefits that help pay for personal care supports. Eligibility, application steps, and benefit levels differ across programs, so families should consult program administrators or a benefits counselor to see what applies. Many households combine public benefits with private‑pay solutions to cover full‑time care. Understanding these funding paths helps you build a sustainable mix of resources; the next subsection outlines key Pennsylvania rules for live‑in caregiver arrangements.
What Are the Pennsylvania Regulations for Live‑In Caregivers?
Pennsylvania rules address wage and hour issues, sleep‑break policies, and employer responsibilities that matter when families hire live‑in caregivers — especially for private hires or household employers. Key considerations include documenting written agreements that clarify work hours and sleep expectations, complying with payroll and tax obligations when acting as an employer, and ensuring minimum wage and overtime requirements are met where applicable. Families should consult state labor resources or an eldercare advisor as needed to ensure compliance and protect both caregiver and client. Clear documentation and following regulations also reduce misunderstandings and support longer caregiver retention.
When you’re ready to evaluate options and get a tailored recommendation, Home Matters offers complimentary consultations and free assessments to match needs, safety indicators, and budget to the right in‑home care model.
1. Next steps: Start with a needs assessment and document nighttime behaviors and medical complexity. 2. Trial options: Consider short trial periods or hybrid coverage to test fit before committing long term. 3. Professional support: Involve medical professionals or a care manager for complex cases to ensure safety and regulatory compliance.
1. Document current care gaps: Note nighttime incidents and medication complexity. 2. Compare models and costs: Use the tables and checklists above to match needs with realistic budgets. 3. Schedule a consultation: Request an assessment to build a concrete, localized care plan.
1. Assess safety first: Prioritize options that close immediate risk gaps. 2. Balance continuity and cost: Where feasible, combine live‑in continuity with supplemental overnight coverage. 3. Leverage available benefits: Explore Medicaid waivers and VA benefits early to reduce private‑pay burden.
For personalized guidance, a free assessment from Home Matters can clarify which service model best fits your loved one’s clinical needs and your household budget.
1. Prepare documentation: Bring medication lists, recent hospital records, and notes on nighttime behaviors. 2. Identify household constraints: Note home layout features that may affect caregiver response. 3. Plan a monitoring strategy: Decide on trial periods, regular check‑ins, and review timelines to reassess fit.
These planning steps make transitioning to either 24‑hour or live‑in care more manageable and measurable.
This article has explained operational definitions, cost considerations, decision checklists, specialized‑care guidance, and Pennsylvania‑specific regulatory and program context to help Philadelphia families choose between 24‑hour home care and live‑in care. If you’d like a recommendation tailored to your loved one’s clinical profile, Home Matters offers free assessments and consultations to support next steps.
Frequently Asked Questions
What is the difference between 24‑hour care and live‑in care in terms of caregiver availability?
Twenty‑four‑hour care uses multiple caregivers in shifts so someone is awake and available around the clock. That ensures an awake responder for emergencies at any hour. Live‑in care usually involves a single caregiver living on‑site who provides daytime assistance and takes scheduled sleep breaks at night. That proximity can be helpful, but it doesn’t guarantee the same level of immediate overnight response as awake‑shift coverage.
How can families assess the suitability of 24‑hour care versus live‑in care for their loved ones?
Start with a thorough needs assessment that looks at medical conditions, cognitive status, mobility, and nighttime behaviors. Determine whether the person needs constant supervision or help with complex medical tasks. Then factor in your budget and the home environment. A care manager, social worker, or clinician can help translate clinical needs into a recommended care model.
Are there specific training requirements for caregivers in 24‑hour care versus live‑in care?
Yes. Caregivers in 24‑hour models often receive specialized training for complex medical needs and dementia care; agencies usually provide training in emergency response, medication management, and behavioral strategies. Live‑in caregivers also benefit from training, though the emphasis is often on daily living assistance and building consistent routines. Always ask providers about specific qualifications and training before you hire.
What role do family members play in the care process when opting for 24‑hour or live‑in care?
Family members are central in both models: they offer emotional support, help make decisions, and sometimes assist with daily tasks. With 24‑hour care, families may coordinate across multiple caregivers and monitor care plans. With live‑in care, families often build a closer relationship with a single caregiver, which can improve continuity. Open, regular communication between family and caregiver is essential in either arrangement.
How do local regulations impact the hiring of live‑in caregivers in Philadelphia?
Pennsylvania and local rules influence wage standards, overtime pay, and sleep‑break policies for live‑in caregivers. Families who hire privately should have written agreements that outline hours and responsibilities and should understand payroll and tax obligations if they act as an employer. Consult state labor resources or an eldercare advisor to make sure you comply with regulations and protect both caregiver and client.
What are some common misconceptions about live‑in care?
A common misconception is that live‑in care is always cheaper than 24‑hour care. While it can be more affordable in many cases, live‑in arrangements may not provide the same overnight supervision that some clients need. Another misconception is that live‑in caregivers are available every minute — they require scheduled rest, and response times at night may be limited. Evaluate needs carefully before assuming cost equals suitability.
How can families ensure a smooth transition to either 24‑hour or live‑in care?
Begin with a comprehensive needs assessment and involve clinicians as needed. Set clear expectations with caregivers about routines and responsibilities. Consider trial periods to test fit, and schedule regular check‑ins and adjustments based on feedback. That approach helps catch issues early and ensures the care arrangement meets evolving needs.