Personal Care Assistance in Philadelphia: A Practical Guide for Families
Personal care assistance in Philadelphia helps older adults and people with disabilities stay safe and independent at home while giving families reliable, practical support. This guide breaks down what personal care assistance (PCA) covers, how it differs from medical home health, and why in-home PCA focuses on Activities of Daily Living (ADLs) and Instrumental Activities of Daily Living (IADLs). You’ll find guidance on matching needs to hours of care, comparing local providers, and estimating realistic costs. We also cover caregiver qualifications in Pennsylvania, clear cost scenarios and funding options, dementia-capable and respite services, neighborhood resources around Philadelphia, and simple actions families can take to support a loved one receiving care. Throughout, the goal is practical: checklists, interview prompts, sample scenarios, and local tips so you leave ready to arrange safe, respectful in-home personal care.

What Are Personal Care Services and Activities of Daily Living in Philadelphia?
In Philadelphia, personal care assistance means non-medical, in-home help with everyday tasks that affect hygiene, mobility, nutrition, and safety. Trained personal care assistants use hands-on support and consistent routines to lower fall risk, slow functional decline, and help people remain independent — which can also reduce hospital readmissions. Practically speaking, PCA covers ADLs (core physical needs) and IADLs (household and community tasks) that keep someone living at home. Knowing the difference helps families decide whether a loved one needs a few companion hours, several daily personal care visits, or a higher-intensity plan that blends ADL and IADL help.
Below are the common ADLs and IADLs, with examples you can use to identify needs and prioritize care.
- Bathing and showering: Help with safe transfers, washing, and grooming to lower fall and skin-care risks.
- Dressing: Assistance picking and putting on clothes safely, and managing adaptive garments when needed.
- Toileting and continence care: Support with transfers, incontinence care, and preserving dignity.
- Transferring and mobility: Safe moves in and out of bed or chairs and steadying while walking, using belts or devices.
- Eating and feeding: Meal setup, cueing, or hands-on feeding when required to maintain nutrition.
- Personal hygiene: Grooming, oral care, and skin care to prevent infections and support wellbeing.
These ADL examples show when hands-on PCA is needed and when to consider medical home health for clinical care. A clear ADL assessment often helps determine recommended hours of in-home personal care services.
Which Activities of Daily Living Does Personal Care Assistance Cover?
Personal care assistants in Philadelphia commonly support the six core ADLs that directly affect daily safety and independence. Care is delivered through consistent, practical routines tailored to each person’s abilities. For example, a PCA may help a newly homebound senior with safe transfers and supervised bathing to prevent falls, or provide step-by-step dressing help for someone with limited range of motion. Caregivers also support nutrition by preparing bite-size foods and offering feeding assistance for people with swallowing issues, while coordinating concerns with clinicians as needed. If one ADL starts to decline, that’s usually a sign to reassess care intensity and consider adding hours or specialist services.
Spotting patterns — whether one task or several are changing — helps families estimate visits needed and decide if short-term training for caregivers or family members might restore function. The next section explains IADLs and how they complement ADL support to keep people safe at home.
What Are Instrumental Activities of Daily Living and How Do They Support Seniors?
IADLs are household and community tasks that make independent living possible. In-home personal care IADLs usually include meal preparation, light housekeeping, medication reminders, grocery shopping, bill organization help, and rides to appointments. When a PCA handles IADLs, it reduces isolation, improves medication adherence through reminders, and prevents hazards by keeping the home safe. Strong IADL support can be the difference between temporary extra help and a long-term care move: it preserves function and lowers family caregiver stress.
Prioritize IADLs by frequency and safety impact — meal prep, medication reminders, and transportation often give the biggest returns in wellbeing and independence.
Differentiate core personal tasks from household activities to match services with needs:
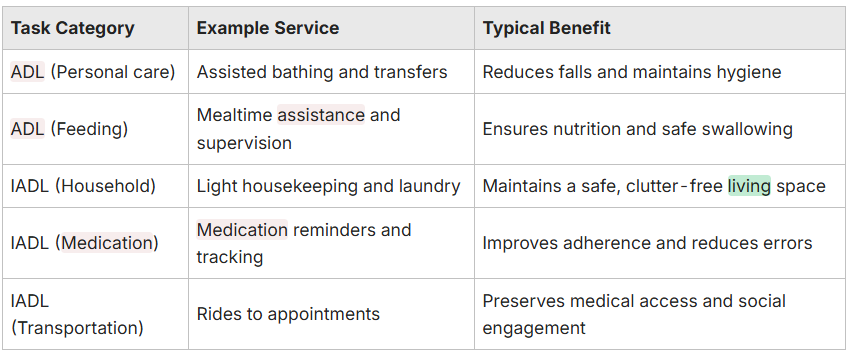
This table clarifies which tasks are hands-on personal care versus household supports so families can build a complete in-home support plan and better estimate hours and provider fit.
How to Choose the Right Personal Care Assistance Provider in Philadelphia?

Picking the right PCA provider means checking staff qualifications, background screening, scheduling reliability, and how well the agency tailors plans to Philadelphia neighborhoods. A strong provider clearly explains the scope — what PCA covers and what needs a licensed home health clinician — then matches caregivers by skill, language, and cultural fit. Ask about contingency plans for staffing gaps, communication routines, and how care is tracked and updated. Local proximity matters: a nearby caregiver can cut travel time, improve punctuality, and make better neighborhood referrals.
Start with a list of non-negotiables, then interview agencies or vetted independent PCAs using the same questions so you can compare answers fairly. The sections below list recommended qualifications to verify and the key questions to ask during meetings.
What Qualifications and Training Should Philadelphia Caregivers Have?
Reliable Philadelphia personal care assistants show competency with background checks, training in safe transfers and infection control, and dementia-capable education when caring for cognitive impairment. Families should confirm criminal background screening, reference checks, and basic certifications like first aid/CPR. Ongoing in-service training — on behavioral strategies, medication reminder protocols, and fall prevention — signals quality. Specialized dementia training and strong family communication skills improve outcomes and caregiver confidence. Ask how the provider reassesses competence and what supervision or clinical oversight they offer to keep skills consistent.
Verifying initial qualifications and ongoing training reduces risk and shows the provider’s commitment to person-centered care. The next section offers prioritized interview questions to use when evaluating agencies and caregivers.
Which Questions Should Families Ask When Selecting a Home Care Agency?
When interviewing agencies or independent PCAs, focus on questions that reveal scope, safety practices, and communication so you can compare responses clearly. Use this checklist during meetings to capture consistent answers and evaluate fit.
- What services are included in personal care assistance and what requires a licensed clinician?
- How do you screen and vet caregivers, including background checks and references?
- What training do caregivers receive, and is dementia-capable training standard?
- How are schedules managed and what is your plan for staff absences or overtime?
- How is the care plan created, documented, and updated with family input?
- What are your billing, cancellation, and overtime policies?
- How do you communicate with families about changes, incidents, or progress?
- Can you provide neighborhood-specific references or examples of local resources you use?
Use these questions to compare agencies on transparency and person-centered practices; a dependable provider will answer directly and offer concrete examples. After you confirm answers, you can weigh cost and funding options described in the next section.
Weigh whether an agency’s oversight or a vetted independent PCA better fits your family’s priorities — each has trade-offs in flexibility, accountability, and cost. If you’re ready to move forward, the next section reviews typical costs and funding pathways in Pennsylvania.
Tip: ask providers how they personalize PCA plans and invite a trial visit so you can see care in action.
What Are the Costs and Funding Options for Personal Care Assistance in Philadelphia?
Costs for personal care assistance in Philadelphia depend on care intensity, number of visits, and whether dementia-capable support is needed. Most in-home PCA is billed hourly; evenings, weekends, travel time, and specialty training can raise rates. Cost drivers include ADL complexity (hands-on transfers versus reminders), nightly checks, whether two caregivers are required for safe transfers, and involvement of agency supervision or a licensed clinician. Build sample monthly budgets from realistic weekly hours and include contingencies for overtime, holiday premiums, and agency administrative fees.
Below are sample scenarios showing service levels, hourly intensity, and estimated monthly costs to illustrate how needs translate into out-of-pocket spending and potential funding sources.
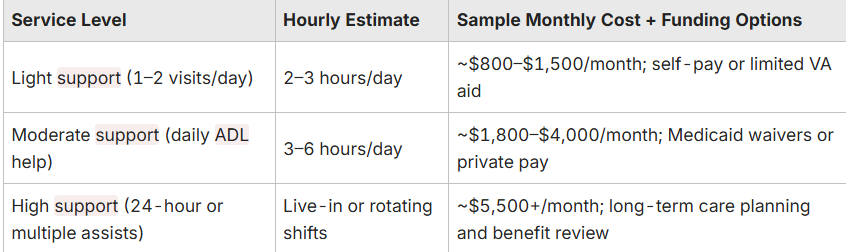

This comparison shows how different need levels map to likely monthly costs and which public or private funding streams to explore. The following section explains typical hourly ranges and how to convert your chosen service level into a household budget.
How Much Does In-Home Personal Care Typically Cost in Philadelphia?
In-home personal care in Philadelphia usually follows hourly pricing and varies with local demand and care complexity. Light companion and IADL support (2–3 hours daily) produces lower monthly totals, while full ADL support — with transfers and bathing assistance — increases hours and cost, especially when two caregivers are needed. Factors that bump prices include night checks, weekend care, dementia training, and rapid start after hospital discharge.
To budget, multiply your expected hourly rate by weekly hours, then add a 10–20% contingency for overtime or extra visits during illness. Discuss scenarios with providers so quotes reflect likely changes in service intensity and avoid surprises when needs shift.
What Financial Assistance and Insurance Options Are Available for PCA?
Families should know Medicaid waivers in Pennsylvania, some VA benefits, and certain long-term care insurance policies can offset PCA costs. Medicare generally covers medically necessary home health services, not non-medical PCA. Local aging services and Area Agencies on Aging can help screen for benefits and point to grant-funded respite or limited-aid programs. Talk with a benefits specialist or social worker for eligibility checks and apply early — approval timelines can affect when care can begin.
Build a prioritized funding checklist: confirm Medicaid/waiver eligibility, check VA or veteran-directed care if applicable, review long-term care insurance riders, and plan short-term private-pay coverage while benefits are pending. Clear budgeting and early benefit navigation reduce the risk of interrupted care.
What Specialized Personal Care Services Are Available for Seniors in Philadelphia?
Specialized personal care services extend beyond routine ADLs and IADLs to meet needs like dementia support, post-hospital recovery, or caregiver respite. These services combine targeted training, simple environmental changes, and structured activities — such as memory-friendly routines and meaningful engagement — to lower behavioral episodes and support recovery. Specialized caregivers are trained in consistent cueing, safe wandering prevention, and family coaching, helping households adapt to changing needs. Ask providers for documented specialized training, a structured care plan, and coordination with clinicians for complex transitions.
Below is a comparison of specialized service types and what families can expect from each to help you decide which supports to request.
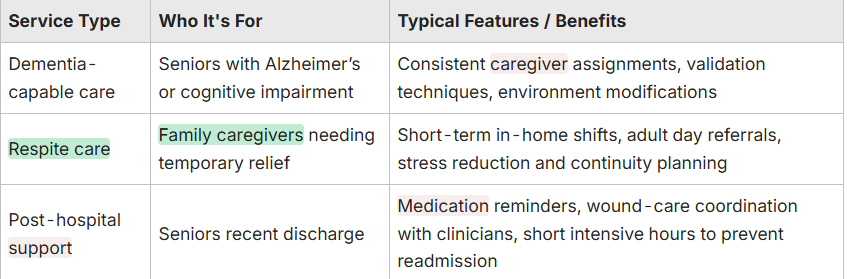
This comparison helps families match specialized services to their situation and prepare to ask for specific training or written protocols when hiring caregivers. The sections below describe dementia care and respite planning in more detail.
How Does Dementia and Alzheimer’s Home Care Support Philadelphia Families?
Dementia-capable home care emphasizes predictable routines, calm communication, and small environment changes that reduce anxiety and preserve dignity. Care plans rely on consistent staffing to build trust, simple cues for daily tasks, and respectful strategies to prevent wandering — such as discreet redirection or safety measures. Caregivers trained in behavior management and trigger recognition can lower incidents and help families reinforce routines. Coordinated care that aligns PCA activities with clinician recommendations and community memory programs usually produces better outcomes and can slow functional decline.
Ask for examples of specific dementia training and real-life approaches caregivers have used with challenging behaviors — practical experience matters more than vague promises.
What Is Respite Care and How Does It Help Family Caregivers?
Respite care gives family caregivers planned relief through in-home shifts, adult day programs, or short residential stays so they can rest, handle appointments, or work without sacrificing their loved one’s routine. Good respite includes a trial visit to build rapport, clear medication and routine instructions, and a defined handoff with contingency plans. The benefits are clear: less stress, better sleep, and improved ability to continue caregiving long term.
When arranging respite, choose providers with written handover procedures and clear care notes so you return to a stable, familiar routine.
How Can Families Support Their Loved Ones with Personal Care Assistance in Philadelphia?
Families are central to planning, coordinating, and emotionally supporting a loved one who receives in-home personal care. Start with a written, personalized care plan that lists ADL/IADL needs, preferred routines, emergency contacts, and measurable goals for safety and function. Schedule regular check-ins, keep shared care notes, and divide responsibilities among family members to reduce confusion and ensure consistent care. Adding small social activities and neighborhood engagement in the plan supports emotional wellbeing and counters isolation.
Practical help includes keeping an up-to-date medication list and allergy information, preparing the home for safe transfers, and sharing the person’s history and preferences with caregivers. Small gestures of appreciation for caregivers — like a thank-you note or a local treat — build goodwill. Local businesses can offer thoughtful tokens families use to acknowledge caregivers or mark milestones while supporting neighborhood shops.
Tip: work with your provider to personalize the PCA plan around daily routines and meaningful activities for your loved one.
What Legal and Financial Considerations Should Families Know About Senior Care?
Key legal and financial steps for senior care include establishing power of attorney, advance directives, and reviewing benefits to understand coverage for in-home services and long-term care. A financial power of attorney lets someone manage bills and pay for care; a healthcare proxy and advance directive document medical wishes if the person cannot decide. Financial planning may include arranging account access for caregiver payments, checking Medicaid waiver or veteran benefit eligibility, and protecting assets with professional advice. Families should consult Philadelphia elder law attorneys or financial planners for tailored guidance.
Start by gathering insurance policies, bank statements, and current legal documents so advisors can give specific recommendations; early planning avoids rushed decisions after a crisis.
Where Can Philadelphia Families Find Support Groups and Community Resources?
Philadelphia families have access to Area Agencies on Aging, caregiver support groups, community centers, and veteran services that offer education, respite referrals, and neighborhood programs to support seniors. Look for local memory cafés, adult day programs, and faith-based volunteer networks that supplement in-home PCA and reduce isolation. Neighborhood senior centers and community health outreach often provide practical help like transportation, benefits application assistance, and social activities tailored to different Philadelphia communities. Regularly connecting with these groups gives emotional support, practical referrals, and peer strategies that complement paid care. For additional comprehensive information and tools, families can also explore dedicated online resources.
When researching resources, ask for neighborhood-specific referrals and check for sliding-scale fees or short-term grants that can help with respite and care transitions. Keep a list of contacts and referral steps in the care plan for quick access when needs change.
Tip: include community contacts and support-group meeting times in your written care plan so everyone knows where to turn.
What Are the Benefits of In-Home Personal Care Assistance for Philadelphia Seniors?
In-home personal care assistance helps seniors stay in familiar surroundings while getting tailored support for daily tasks and social connection. PCA reduces fall risk through safe transfers, improves nutrition with meal help, and supports medication adherence through reminders and monitoring — all of which can reduce emergency visits and better manage chronic conditions. Emotional benefits include steady companionship and less family caregiver burnout when responsibilities are shared with trained professionals. Overall, PCA blends practical help with dignity-preserving routines that reflect the person’s preferences.
Families gain lower stress and more ability to keep working or manage other responsibilities, while seniors get predictable supports that let them do meaningful activities. The sections below explain specific ways PCA improves function and how families can get peace of mind.
How Does PCA Improve Quality of Life and Maintain Senior Independence?
PCA targets functional gaps with focused interventions — gait techniques for safer walking, adaptive tools for dressing, and meal plans that meet dietary needs — to sustain autonomy. Regular help prevents small issues from becoming hospital problems by ensuring hygiene, nutrition, and medication are managed on time; this is especially valuable after a hospital stay or during disease flare-ups. PCA also enables ongoing social participation through transportation and outings, which supports mental health and cognition. Set measurable goals in the care plan — for example, safer transfers or independent dressing — to monitor progress and adjust care.
Tracking outcomes and celebrating small wins shows the value of PCA and guides decisions about increasing or tapering support as needs change.
How Does Personal Care Assistance Provide Peace of Mind for Families?
PCA offers peace of mind through regular monitoring, clear communication, and written care plans that create predictable routines and accountable care. Scheduled updates, written care notes, and periodic plan reviews keep families informed about changes and allow timely adjustments, easing worry about unattended needs. Respite options and shared caregiving responsibilities reduce burnout and make long-term support sustainable without sacrificing work or health. Simple practices — weekly summaries, emergency protocols, and shared goal-setting — help families stay involved while delegating daily tasks to trained professionals.
To build trust, insist on clear reporting and periodic outcome reviews tied to specific goals — that turns daily care into measurable reassurance.
Tip: ask for a weekly summary note and a short monthly review to track progress and maintain communication.
Frequently Asked Questions
What is the difference between personal care assistance and home health care?
Personal care assistance (PCA) provides non-medical help with daily living tasks like bathing, dressing, and meal prep. Home health care is medical care delivered by licensed clinicians — nurses, therapists, or other professionals — for clinical needs. Use PCA when the priority is safe daily support and independence; choose home health when skilled medical treatment is required.
How can families assess the quality of personal care services?
Check caregiver qualifications, read reviews, and ask for local references. Observe caregiver interactions during an initial visit to assess fit and communication. Ask about the agency’s training, supervision, and emergency procedures — and request concrete examples of how they handle schedule gaps or behavior issues.
What should families include in a personalized care plan?
A good care plan lists ADL and IADL needs, daily routines, emergency contacts, medications and allergies, and measurable goals for function and safety. It should also spell out communication preferences between family and caregivers and be updated regularly as needs change.
Are there specific training programs for caregivers in Philadelphia?
Yes. Many local agencies provide specialized training in dementia care, fall prevention, and communication strategies, plus certifications like CPR and first aid. Ask providers for details on ongoing education and documented competency checks.
How can families ensure continuity of care when a caregiver is unavailable?
Discuss contingency plans with the agency: ask how they cover staff absences, whether they provide backup caregivers, and how they notify families. A clear communication channel and written handover notes help keep routines steady when staff change.
What role do community resources play in supporting personal care assistance?
Community resources extend PCA by offering transportation, meal delivery, social activities, and benefit navigation. Area Agencies on Aging, local senior centers, and caregiver support groups provide referrals, respite options, and neighborhood-based programs that complement paid care.
How can families participate in the care process without overwhelming themselves?
Divide duties among family members, set regular check-ins, and use shared care notes to keep everyone informed. Prioritize self-care and lean on community resources or respite services to avoid burnout while staying involved in decision-making.